| |
Once accepted into an accredited chiropractic college, the requirements become even more demanding — four to five academic years of professional study are the standard. Because of the hands-on nature of chiropractic, and the intricate adjusting techniques, a significant portion of time is spent in clinical training.
Doctors of chiropractic — who are licensed to practice in all 50 states, the District of Columbia, and in many nations around the world — undergo a rigorous education in the healing sciences, similar to that of medical doctors. In some areas, such as anatomy, physiology, and rehabilitation, they receive more intensive education than most medical doctors or physical therapists.
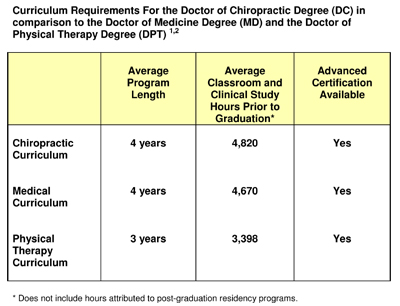
Like other primary health care doctors, chiropractic students spend a significant portion of their curriculum studying clinical subjects related to evaluating and caring for patients. Typically, as part of their professional training, they must complete a minimum of a one-year clinical-based program dealing with actual patient care. In total, the curriculum includes a minimum of 4,200 hours of classroom, laboratory and clinical experience. The course of study is approved by an accrediting agency which is fully recognized by the U.S. Department of Education. This has been the case for more than 25 years. |
|
 |
Before they are allowed to practice, doctors of chiropractic must pass national board examinations and become state-licensed. Chiropractic colleges also offer post-graduate continuing education programs in specialty fields ranging from sports injuries and occupational health to orthopedics and neurology. These programs allow chiropractors to specialize in a healthcare discipline or meet state re-licensure requirements.
This extensive education prepares doctors of chiropractic to diagnose health care problems, treat the problems when they are within their scope of practice and refer patients to other health care practitioners when appropriate.
All About Spinal Decompression Therapy
Spinal Decompression Therapy involves stretching the spine, using a traction table or similar motorized device, with the goal of relieving back pain and/or leg pain.
This procedure is called nonsurgical decompression therapy (as opposed to surgical spinal decompression, such as laminectomy and microdiscectomy).
This article provides an overview of nonsurgical spinal decompression therapy and its role in treatment of lower back pain and neck pain.
Spinal decompression devices use the same basic principle of spinal traction that has been offered by chiropractors, osteopaths, and other appropriately trained health professionals for many years.
Both traction and decompression therapy are applied with the goals of relieving pain and promoting an optimal healing environment for bulging, degenerating, or herniated discs.
- See What's a Herniated Disc, Pinched Nerve, Bulging Disc...? and What Is Degenerative Disc Disease?
Spinal decompression is a type of traction therapy applied to the spine in an attempt to bring about several theoretical benefits including:
- Create a negative intradiscal pressure to promote retraction or repositioning of the herniated or bulging disc material.
- Create a lower pressure in the disc that will cause an influx of healing nutrients and other substances into the disc.1
Article continues below
Clinical Evidence
While the fundamental theory of spinal decompression is widely accepted as valid, there is a lack of evidence supporting decompression therapy as being efficacious. Additionally there are some potential risks.
Although some studies that do not include control groups conclude that decompression therapy is efficacious, the few that do generally conclude that mechanized spinal decompression is no better than sham decompression. [Schimmel JJ, et al. European Spine Journal 18(12):1843-50, 2009] Thus, there is insufficient evidence that spinal decompression therapy is as effective, or more effective, than less expensive manual methods in treating back pain or injured herniated discs.2
- See Manual Physiotherapy for Pain Relief
A review of medical literature to date indicates that most clinical trials examining the efficacy of spinal decompression therapy or traction were lacking in one or more areas, such as inadequate numbers of subjects to make a statistically valid conclusion, lack of blinding (the patient or provider is unaware of the treatment given), no comparison to a placebo group (called a sham controlled study), or lack of comparison to a treatment alternative.3 At the time of this article, few clinical studies of spinal decompression therapy have been published in peer reviewed medical journals.
- Research and locate chiropractors in your area that can help alleviate your back and neck pain.
Understanding Spinal Manipulation
There are well over 100 types of adjustment techniques used by chiropractors throughout the world. Typically, chiropractors will focus on and utilize 8 to 10 different approaches in their practice.
The common goal of most chiropractic techniques is to restore or to enhance joint function, with the general goals of resolving joint inflammation and reducing pain. Some approaches use some force (spinal manipulation), while others are more gentle (spinal mobilization).
- See Chiropractic Adjustment
The original chiropractic adjustment approach is generally referred to as spinal manipulation, and may also be called the diversified technique or the high-velocity, low-amplitude (HVLA) thrust. New chiropractic adjustment approaches typically evolve as a variation from an existing technique and are often named after the chiropractor who developed it.
- See Chiropractic Adjustment of the Lumbar Spine (Low Back) Video
This article reviews a number of the most commonly used spinal manipulation and spinal mobilization techniques currently used by chiropractors.
Article continues below
Chiropractic Manipulation Techniques
Chiropractors adapt treatment plans to meet the specific needs of each patient. Typically, chiropractic treatment plans involve some forceful and less forceful spinal adjustment techniques during the same visit or over the course of treatment (6 to 10 visits for a typical patient).
Spinal Manipulation (High-Velocity Low-Amplitude Thrust)
The most frequently used chiropractic technique, spinal manipulation, is the traditional high-velocity low-amplitude (HVLA) thrust. The manipulation often results in an audible "pop," as chiropractors use their hands to apply a controlled sudden force to a joint while the body is positioned in a specific way.
Spinal Mobilization (Low-Force or Gentle Chiropractic Techniques)
Some conditions (such as osteoporosis), pathology, the patient's size, patient comfort, or patient preference, may require a gentler approach generally referred to as spinal mobilization. In addition, some patients and/or clinicians prefer mild spinal mobilization techniques that do not involve twisting of the body or a forceful thrust.
In addition to manipulation, many chiropractors will employ adjunctive therapy, such as ice or heat or Physiotherapy modalities (such as electric stimulation, ultrasound, etc.), as part of an overall treatment plan. Patients should discuss their symptoms and preferences with their chiropractor, whose role it is to perform a thorough examination to determine the best course of treatment.
- See Chiropractic Treatments for Lower Back Pain
Chiropractors are not the only health care providers who utilize spinal manipulation for back pain treatment. Many osteopathic physicians will provide a variety of types of spinal adjustments, such as the spinal manipulation and mobilization described in this article. Occasionally, other types of health care professionals, such as physical therapists or physiatrists, will be trained in providing spinal manipulation as well.
- See How To Select The Best Chiropractor
Research and locate chiropractors in your area that can help alleviate your back and neck pain.
Living with Osteoarthritis
What Is Osteoarthritis?
Osteoarthritis (OA), or degenerative joint disease, affects more than 20 million Americans and is more common in women than in men. The disease affects the cartilage—slippery tissue on the ends of bones that meet in a joint. Normally, cartilage helps bones glide over one another. In an OA patient, however, the cartilage is broken down and eventually wears away. As a result, instead of gliding, bones rub against each other, causing pain, swelling, and loss of motion.
Although the majority of patients with OA are 65 and older, recent research shows that osteoarthritis is not a by-product of aging. Family history of OA, being overweight, lack of exercise, and prior joint injuries are suggested as OA risk factors.
How Is Osteoarthritis Diagnosed?
OA is diagnosed through a combination of clinical history, patient examination, and x-rays. Other tests, such as drawing fluid from the joint, are sometimes used.
The signs of OA include:
• Steady or intermittent joint pain
• Joint stiffness after sitting, sleeping, or otherwise not moving for a long time
• Swelling or tenderness in the joints
• A crunching feeling or the sound of bones rubbing against each other.
Should Osteoarthritis Patients Exercise?
Exercise is one of the best forms of OA treatment—and prevention. It strengthens the muscular support around the joints and improves and maintains joint mobility and function. In addition, exercise helps to control weight and improve the patient’s mood and outlook—important factors influencing the severity of the symptoms.
If you suffer from OA, consider the following exercise tips:
• Low-impact or non-weight-bearing activities, such as walking, stationary training, and light weight training work best for OA patients.
• Use strengthening exercises if the key muscle groups that relate to the function of the joints are weakened by the degeneration.
• If you are overweight, start exercising carefully, so as not to put too much stress on the knee and ankle joints.
• Stair climbing, water aerobics, Theraband workouts, and similar exercises will help to keep the joints mobile without straining them.
• Learn to read the body’s signals and know when to stop, slow down, or rest.
How Can Your Chiropractor Help?
Doctors of chiropractic, by the nature of their work, can detect the earliest degenerative changes in the joints. They see the impact of degenerative changes in the spine, as well as in the hips, knees, and other weight-bearing joints. Doctors of chiropractic are also trained to relieve the pain and improve joint function through natural therapies, such as chiropractic manipulation, trigger-point therapy, or some massage techniques.
Doctors of chiropractic can provide exercise counseling, helping you choose exercises that are best for you. If a sore or swollen joint prevents you from exercising, talk to your doctor of chiropractic about other drug-free pain-relief options, such as applying heat or cold to the affected area. In addition, your doctor of chiropractic can help you choose proper supplements that play important roles in OA prevention and treatment.
|
|





